Peyronie’s disease is a condition where scar tissue causes the penis to curve or lose length or girth. In some cases, it can cause pain and prevent the man from having sex.
There are surgical and nonsurgical treatments that can manage it and it doesn’t cause any harm to the rest of the body.
The information below is intended to provide responses to many of the common questions men have about Peyronie’s disease when they contact the Kelowna Precision Sexual Health Clinic for men for information or assessment.
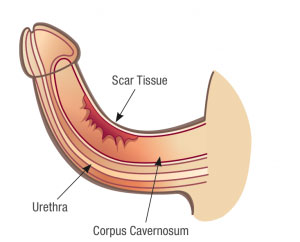
Peyronie’s is a disease where scar tissue in your penis causes it to bend, curve or lose length or girth. You may be able to feel the scar tissue (plaque) through the skin or you may have pain in a specific part of your penis as the scar tissue forms. During an erection, your penis can bend up, down, or to the side depending on the location of the scar. Some men with this condition don’t have a curve, but might have an area of indentation or “hourglass” appearance.
Most men don’t have perfectly straight erections. Just because there is a little curve in your penis, that doesn’t mean you have Peyronie’s disease. Men who have had a curvature their whole lives do not have Peyronie’s disease.
In most cases, the scar forms on the top of the penis, causing it to curve upwards when it becomes erect. Your penis will bend downward if the scar is on the bottom, and sideways if the scar is on the side. In some cases, the scar develops on both the top and bottom of the shaft, which can cause the penis to become “dented” or shorter. Sometimes the scar will go all the way around the penis, making it narrow like the neck of a bottle or the center of an hourglass. About one in three men with this condition may have calcium in the scar tissue that can make it feel like bone.

Peyronie’s disease has two stages: acute and chronic.
Acute phase: This stage lasts between six and 12 months. During this period the scar forms under the skin of your penis, causing a curvature or other change in its shape. You may feel pain when your penis is erect or when it is soft.
Chronic phase: The scar has stopped growing in this phase, so the curvature in the penis doesn’t get worse. The pain will usually be gone by this time, but sometimes it can continue, especially with erections. Also, erectile dysfunction (ED) or problems getting or keeping the penis hard may develop.
Several risk factors might increase your chances of getting Peyronie’s disease:
Age. Peyronie’s disease is more likely to happen as you get older. It occurs in about 10-15% of middle-aged men.
Genetics. If you have a close relative (brother or father, for example) with the disease, you’re at a higher risk.
Connective tissue disorders. Those with a connective tissue disorder are at a greater risk. Examples of those disorders include Dupuytren’s disease, plantar fasciitis and scleroderma.
Erectile dysfunction. Men who have diabetes-associated erectile dysfunction (ED) (impotence/difficulty getting and keeping an erection) are four to five times more likely to develop Peyronie’s disease. Sometimes erectile dysfunction can be caused by having Peyronie’s.
Prostate cancer. Men who have had surgery for prostate cancer are at an increased risk.
Autoimmune disorders. If you have an autoimmune disorder like lupus, you’re more likely to get Peyronie’s disease.
It is recommended to go to the doctor for a diagnosis. It is normal to feel embarrassed but doctors are used to dealing with problems such as this. The sooner you get diagnosed, the sooner you can get treatment. Most professionals recommend starting some form of Peyronie’s treatment during the acute phase and ideally within 6 months of noticing the first symptoms.
It is estimated that Peyronie’s disease improves or resolves without any treatment in only 5 – 15% of cases.
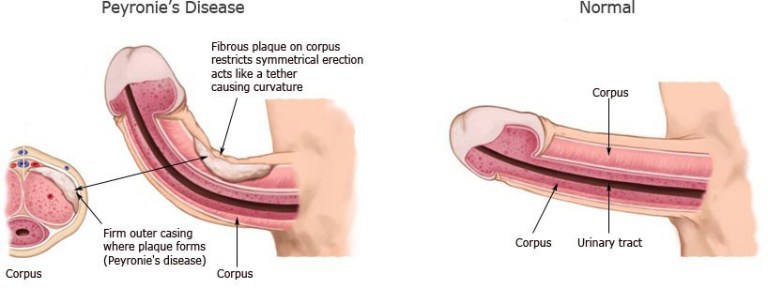
There are a number of treatment options. Some work well for some men but not for others. Starting a non-surgical treatment as soon as possible is a good idea.
The aim of most treatments is to stop the disease progressing further, maintain or improve sexual function, relieve any penile pain and to straighten the bend as much as possible.
Many modalities have been tested in Peyronie’s disease and have found to be effective. These include intralesional therapies (penile injections), oral therapies, topical therapies, penile traction devices, low-intensity acoustic shockwave, and surgical procedures.
Please see the treatments offered at our Regina and Saskatoon clinics.
Revibe Regina
2075 Prince of Wales Dr., Suite 215
Regina, SK S4V 3A3
Revibe Saskatoon
303 Wellman Lane, Suite 303
Saskatoon, SK S7T 0J1
Telephone:
306-373-8423